Clearblue offers a range of home fertility and ovulation products, all of which monitor luteinising hormone (LH) in urine to identify the time of peak fertility. The Clearblue Advanced Fertility Monitor and Clearblue Advanced Digital Ovulation Test also measure E3G (estrone-3-glucuronide), a urinary metabolite of another key female hormone, estrogen, to identify the period of high fertility that occurs prior to the LH surge. Monitoring these two hormone levels helps women identify the fertile days of their cycle enabling them to time intercourse to the days when conception is most likely.
- Clearblue Period and Cycle Tracker App
- Clearblue Advanced Fertility Monitor
- Clearblue Advanced Digital Ovulation Test
- Clearblue Digital Ovulation Test
How urinary LH and E3G can be used to identify fertile days
There are only a few days per cycle when a woman is fertile and can conceive. Evidence shows that this ‘fertile window’ usually spans 6 days, starting approximately 5 days prior to ovulation and ending on the day of ovulation itself.1 The 6-day fertile period is affected by:
-
The lifespan of the egg, which is up to 24 hours after ovulation
-
The lifespan of sperm which is more variable. The median is 1.5 days2, but sperm can generally survive for several days in the sperm supportive mucus3 found in the fertile days of the cycle. Sperm survival is therefore dependent on the type and quantity of the mucus within the cervix, and the quality of the sperm itself.
The two most fertile days of this 6-day fertile window are known as peak fertility days. These peak fertility days are the day prior to ovulation and the day on which ovulation takes place.4
Studies show that a surge in LH level occurs 24-36 hours prior to ovulation,4 and that this LH surge is an accurate and reliable marker of impending ovulation.5-9 The urinary LH surge pinpoints the two peak fertile days of a woman's cycle, with intercourse on these days being shown to be associated with the highest likelihood of conception.1
In the days leading up to the LH surge, estradiol levels rise gradually, reaching a threshold that triggers the pre-ovulatory LH surge. Tracking E3G, the urinary metabolite of estradiol, allows women to identify the days of high fertility leading up to ovulation, where conception is also possible, and this also gives them advanced notice of their peak fertile days. Data shows that women who are aware of their fertile days have an increased likelihood of conceiving.10,11
Furthermore, estradiol stimulates secretion of cervical mucus that is favourable for the survival and transport of sperm. The rise in plasma estradiol corresponds closely to the appearance of sperm-supportive cervical mucus.12 Therefore, intercourse during the 6-day fertile period may lead to conception, as sperm can survive for a number of days.
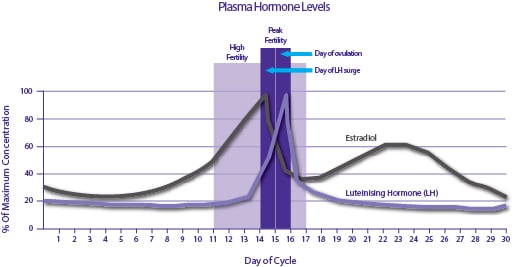
Typical changes in Estradiol and LH during the menstrual cycle.
The Clearblue Fertility Monitor/Clearblue Advanced Fertility Monitor
The The Clearblue Fertility Monitor/Clearblue Advanced Fertility Monitor is a unique innovation proven to increase the chances of conception by 89% over the first 2 cycles of use13 which can help reduce the time it takes to conceive.14 It accurately monitors levels of LH and E3G to typically identify up to 6 days of high and peak fertility per cycle. This makes the Clearblue Fertility Monitor/Clearblue Advanced Fertility Monitor the most advanced home methods of maximising the chance of conception. Clinical studies have found urinary measurements by Clearblue Fertility Monitor/Clearblue Advanced Fertility Monitor closely reflect serum concentrations of the hormones8 and the LH surge detection by the monitor accurately predicts ovulation.7
In addition to reading the dual-hormone assay for fertility hormones on fertility Test Sticks, the Clearblue Advanced Fertility Monitor can read pregnancy Test Sticks, which contain an assay for human chorionic gonadotrophin (hCG), an established and accurate marker for pregnancy. Clearblue Advanced Fertility Monitor also allows the user to input additional data such as dates of intercourse and menses, and displays information from the previous 6 cycles in a summary chart. The Clearblue Advanced Fertility Monitor has a sleek and feminine design with the added benefit of an intuitive touch-screen display.
The Clearblue Advanced Digital Ovulation Test
The Clearblue Advanced Digital Ovulation Test accurately tracks a woman’s personal menstrual cycle to identify a wider fertile window than other home ovulation tests, by tracking the changing levels in the urinary metabolites of E3G and LH. By measuring these 2 hormones, the Clearblue Advanced Digital Ovulation Test typically identifies 4 or more fertile days, 2 more than any other home ovulation test, for more opportunities to get pregnant naturally 15. The Clearblue Advanced Digital Ovulation Test is more than 99% accurate at detecting the LH surge.16 The digital display shows an unmistakable result in the form of a smiley face when a fertile day is detected. Clearblue Advanced Digital Ovulation Test is available as a 10 test pack (1 month supply) or a 20 test pack (2 month supply).
The Clearblue Digital Ovulation Test
The Clearblue Digital Ovulation Test is over 99% accurate in detecting the presence of LH in urine.17 The Clearblue Digital Ovulation Test identifies the two most fertile days by detecting the pre-ovulatory LH surge. It is a simple home ovulation test kit, which provides easy-to-read, easy-to-understand digital results for more accurate reading in consumers' hands.18
Depending on where you live, the Clearblue Digital Ovulation Test may be available in a number of different pack sizes to accommodate the variability in women’s length of cycle. It has been suggested that the use of home ovulation tests to time intercourse for conception can lead to stress. A recent study found no difference in levels of stress between women using digital ovulation tests compared with women who were trying to conceive without any additional aids. 19
This content is provided for general information purposes only.
Always read package inserts of product before use.
- 1 Wilcox AJ, Weinberg CR, Baird DD. Timing of sexual intercourse in relation to ovulation. Effects on the probability of conception, survival of the pregnancy, and sex of the baby. N Engl J Med 1995 Dec 7;333(23):1517-21.
- 2 Weinberg CR and Wilcox AJ. A model for estimating the potency and survival of human gametes in vivo. Biometrics. 1995 Jun;51(2):405-12.
- 3 France JT, Graham FM, Gosling L, Hair P, Knox, BS. Characteristics of natural conceptual cycles occurring in a prospective study of sex preselection: fertility awareness symptoms, hormone levels, sperm survival, and pregnancy outcome. Int J Fertil. 1992 Jul-Aug;37(4):244- 55.
- 4 Ferreira-Poblete A. The probability of conception on different days of the cycle with respect to ovulation: an overview. Adv Contracept 1997 Jun;13(2-3):83-95.
- 5 Corson SL. Self-prediction of ovulation using a urinary luteinizing hormone test. J Reprod Med 1986;31(8 Suppl):760-3.
- 6 Guida M, Tommaselli GA, Palomba S, Pellicano M, Moccia G, Di Carlo C, et al. Efficacy of methods for determining ovulation in a natural family planning program. Fertil Steril 1999;72(5):900-4.
- 7 Behre HM, Kuhlage J, Gassner C, Sonntag B, Schem C, Schneider HP, et al. Prediction of ovulation by urinary hormone measurements with the home use ClearPlan Fertility Monitor: comparison with transvaginal ultrasound scans and serum hormone measurements. Hum Reprod 2000;15(12):2478-82.
- 8 Tanabe K, Susumu N, Hand K, Nishii K, Ishikawa I, Nozawa S. Prediction of the potentially fertile period by urinary hormone measurements using a new home-use monitor: comparison with laboratory hormone analyses. Hum Reprod 2001;16(8):1619-24.
- 9 Guermandi E, Vegetti W, Bianchi MM, Uglietti A, Ragni G, Crosignani P. Reliability of ovulation tests in infertile women. Obstet Gynecol 2001;97(1):92-6.
- 10 Hilgers TW, Daly KD, Prebil AM, Hilgers SK. Cumulative pregnancy rates in patients with apparently normal fertility and fertility-focused intercourse. J Reprod Med 1992 Oct;37(10):864-6.
- 11 Stanford JB, Dunson DB. Effects of sexual intercourse patterns in time to pregnancy studies. Am J Epidemiol 2007 May 1;165(9):1088-95.
- 12 Burger, HG. Estradiol: the physiological basis of the fertile period. Int J Gynecol Obstet 1989; Suppl 1:5-9.
- 13 Robinson JE, Wakelin M, Ellis JE. Increased pregnancy rate with use of Clearblue Easy Fertility Monitor. Fertility and Sterility 2007;87:329-334.
- 14 Robinson JE, Ellis JE. Mistiming of intercourse as a primary cause of failure to conceive: results of a survey on use of a home-use fertility monitor. Curr Med Res Opin 2007;23(2):301-6.
- 15 SPD Data on file. In a study of 87 women, 4 or more fertile days were identified in 80% of cycles using actual cycle length.
- 16 SPD Data on file. Study found >99% agreement with AutoDELFIA reference method in 100 cycles (all cycle had LH surge >40mIU/ml).
- 17 SPD data on file. Clearblue Digital Ovulation Test has been shown to be 99% accurate when compared to a reference method in laboratory studies using urine samples from 123 cycles in which the LH surge was identified by a reference method.
- 18 Johnson S, Ellis J, Godbert S, Ali S, Zinaman M. Comparison of a digital ovulation test with three popular line ovulation tests to investigate user accuracy and certainty. Expert Opin Med Dign 2011;5:467-473.
- 19 Tiplady S, Jones G, Campbell M, Johnson S, and Ledger W. Home ovulation tests and stress in women trying to conceive: a randomized controlled trial. Human Reproduction 2013;28(1):138-151.
Overview of ovulation and planning pregnancy
An overview of ovulation, the hormones that control ovulation, the methods available to women to help identify ovulation, and their utility in planning pregnancy. Includes tracking hormones using an ovulation test or fertility monitor, calendar calculations, apps, basal body temperature and observation of cervical secretions.

